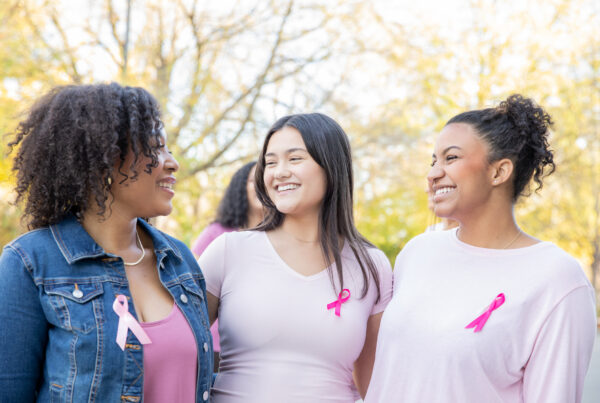by Christian Maino, Graduate Student, University of Illinois
Can you remember the last time you woke up from a restful night of sleep, without the aid of an alarm or of a child requiring attention? This question may evokes a longing for that restful, deep sleep you have not enjoyed for some time. Nearly two-thirds of adults fail to meet the 8-hours of nightly sleep recommended by the National Sleep foundation1. For children 6-13 years, the figure is 9-11 hours of sleep per night, which highlights the vital role sleep plays in promoting healthy development and growth2.
Why do we need sleep?
Scientists warn of the need to increase sleep time and the consequences that poor sleep quality or quantity have on overall health and wellbeing. Research has demonstrated the impact of poor sleep on aspects of metabolic health. An increase in obesity is associated with inadequate sleep4,5. Poor sleep may result in an inclination to overeat and remain sedentary6. The risk of type 2 diabetes, heart disease, and cancer, particularly breast cancer, increases with poorer sleep7–10. Being obese may also cause poor sleep, due to an increased risk of obstructive sleep apnea, which impairs sleep quality11. Poor sleep quality may also be related to an underlying disease. Conditions that cause hormonal imbalances in the body may result in disrupted sleep12,13. The take-away point is that sleep and metabolic health are intricately linked to one another. Most individuals are not able to sacrifice sleep quality or quantity without increasing the risk of debilitating health consequences.
How do we bolster sleep quality and duration?
Experts in the field of sleep biology acknowledge the mismatch of our genetically programmed sleep with the environment of today’s modern world. The biological clock, or the “diurnal cycle” or “circadian rhythm” is what governs the need and desire to sleep at pre-determined times. Our eyes and visual experience relay critical information to a brain structure called the hypothalamus that is responsible for modifying the circadian rhythm. Exposure to ultra-violet, or UV light from the sun signals to the brain that it is daytime. UV light is also what we expose our eyes to when we scroll through our smartphones at night. This exposure prompts neural confusion. You may know that 9 pm is when you have to go to bed, but your body may fight you because it still thinks it is 3 pm! In addition to UV light, chronic stress will also challenge your body’s preprogrammed circadian rhythm.
There are several approaches we can implement to increase sleep quality and duration. Decreasing screen time at night is the first approach to try in order to improve sleep14,15. Other environmental variables to try include:
- Cooling the room temperature, as your body’s ability to cool during sleep is critical16,17.
- Avoiding the use of excessive blankets that may cause overheating.
- Limiting caffeine to only one cup of coffee in the morning max. You may still have caffeine in your bloodstream in the evening from the cup you had in the morning18,19.
- Exercising, especially exercising vigorously in the morning has been shown to promote sleep onset and quality20.
- Going to sleep at the same time each night to establish your biological clock21
- Finishing your last meal well at least a few hours before bedtime, as late-night eating impairs sleep quality22.
Early research shows that incorporating mindful meditation practice before bed may be beneficial for improving sleep quality23. Meditation may take the form of conscious breathing exercises, journaling, or doing another activity that requires diligent attention to one’s actions. Lowering stress levels through such practices can make it easier to fall asleep and stay asleep throughout the night.
The consequences of poor sleep on overall health and wellbeing cannot be overstated. Sleep is vital to proper functioning and wellbeing. We should consider it a tool, as we do with healthy eating, for the prevention of illness.
References
- Hirshkowitz M, Whiton K, Albert SM, et al. National Sleep Foundation’s sleep time duration recommendations: methodology and results summary. Sleep Health. 2015;1(1):40-43. doi:10.1016/j.sleh.2014.12.010
- Guidelines on Physical Activity, Sedentary Behaviour and Sleep for Children under 5 Years of Age. Geneva: World Health Organization; 2019. http://www.ncbi.nlm.nih.gov/books/NBK541170/. Accessed February 29, 2020.
- Cappuccio FP, D’Elia L, Strazzullo P, Miller MA. Sleep Duration and All-Cause Mortality: A Systematic Review and Meta-Analysis of Prospective Studies. Sleep. 2010;33(5):585-592. doi:10.1093/sleep/33.5.585
- Taheri S, Lin L, Austin D, Young T, Mignot E. Short Sleep Duration Is Associated with Reduced Leptin, Elevated Ghrelin, and Increased Body Mass Index. Froguel P, ed. PLoS Med. 2004;1(3):e62. doi:10.1371/journal.pmed.0010062
- Ogilvie RP, Patel SR. The epidemiology of sleep and obesity. Sleep Health. 2017;3(5):383-388. doi:10.1016/j.sleh.2017.07.013
- Chaput J-P, Tremblay A. Insufficient Sleep as a Contributor to Weight Gain: An Update. Curr Obes Rep. 2012;1(4):245-256. doi:10.1007/s13679-012-0026-7
- Knutson KL, Van Cauter E, Rathouz PJ, et al. Association between sleep and blood pressure in midlife: the CARDIA sleep study. Arch Intern Med. 2009;169(11):1055-1061. doi:10.1001/archinternmed.2009.119
- Blask DE. Melatonin, sleep disturbance and cancer risk. Sleep Med Rev. 2009;13(4):257-264. doi:10.1016/j.smrv.2008.07.007
- Cappuccio FP, D’Elia L, Strazzullo P, Miller MA. Quantity and quality of sleep and incidence of type 2 diabetes: a systematic review and meta-analysis. Diabetes Care. 2010;33(2):414-420. doi:10.2337/dc09-1124
- Thompson CL, Larkin EK, Patel S, Berger NA, Redline S, Li L. Short duration of sleep increases risk of colorectal adenoma. Cancer. 2011;117(4):841-847. doi:10.1002/cncr.25507
- Wolk R, Shamsuzzaman ASM, Somers VK. Obesity, Sleep Apnea, and Hypertension. Hypertension. 2003;42(6):1067-1074. doi:10.1161/01.HYP.0000101686.98973.A3
- Shipley JE, Schteingart DE, Tandon R, Starkman MN. Sleep Architecture and Sleep Apnea in Patients with Cushing’s Disease. Sleep. 1992;15(6):514-518. doi:10.1093/sleep/15.6.514
- Trzepacz PT, McCue M, Klein I, Levey GS, Greenhouse J. A psychiatric and neuropsychological study of patients with untreated Graves’ disease. Gen Hosp Psychiatry. 1988;10(1):49-55. doi:10.1016/0163-8343(88)90084-9
- Exelmans L, Van den Bulck J. Bedtime mobile phone use and sleep in adults. Soc Sci Med. 2016;148:93-101. doi:10.1016/j.socscimed.2015.11.037
- Lowden A, Åkerstedt T, Ingre M, et al. Sleep after mobile phone exposure in subjects with mobile phone-related symptoms. Bioelectromagnetics. 2011;32(1):4-14. doi:10.1002/bem.20609
- Muzet A, Ehrhart J, Candas V, Libert JP, Vogt JJ. Rem Sleep and Ambient Temperature in Man. Int J Neurosci. 1983;18(1-2):117-125. doi:10.3109/00207458308985885
- Karacan I, Thornby JI, Anch AM, Williams RL, Perkins HM. Effects of high ambient temperature on sleep in young men. Aviat Space Environ Med. 1978;49(7):855-860.
- Landolt H-P, Rétey JV, Tönz K, et al. Caffeine Attenuates Waking and Sleep Electroencephalographic Markers of Sleep Homeostasis in Humans. Neuropsychopharmacology. 2004;29(10):1933-1939. doi:10.1038/sj.npp.1300526
- Landolt HP, Werth E, Borbély AA, Dijk DJ. Caffeine intake (200 mg) in the morning affects human sleep and EEG power spectra at night. Brain Res. 1995;675(1-2):67-74. doi:10.1016/0006-8993(95)00040-w
- Driver HS, Taylor SR. Exercise and sleep. Sleep Med Rev. 2000;4(4):387-402. doi:10.1053/smrv.2000.0110
- Duffy JF, Kronauer RE, Czeisler CA. Phase-shifting human circadian rhythms: influence of sleep timing, social contact and light exposure. J Physiol. 1996;495 ( Pt 1):289-297. doi:10.1113/jphysiol.1996.sp021593
- Yahia N, Brown C, Potter S, et al. Night eating syndrome and its association with weight status, physical activity, eating habits, smoking status, and sleep patterns among college students. Eat Weight Disord EWD. 2017;22(3):421-433. doi:10.1007/s40519-017-0403-z
- Rusch HL, Rosario M, Levison LM, et al. The effect of mindfulness meditation on sleep quality: a systematic review and meta‐analysis of randomized controlled trials. Ann N Y Acad Sci. 2019;1445(1):5-16. doi:10.1111/nyas.13996
Photo by Ihsan Aditya from Pexels.