Selena Wang, James Scholar Honors project
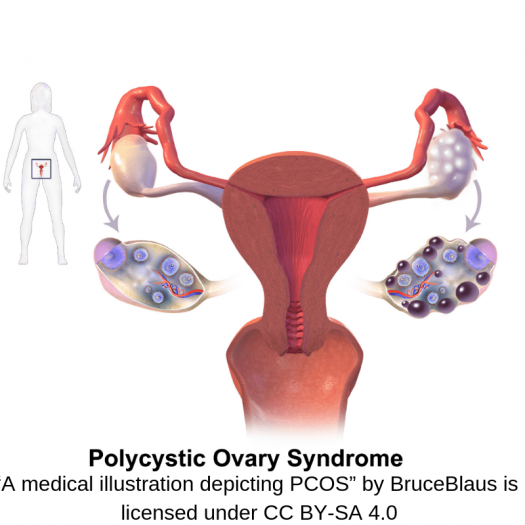
Polycystic ovarian syndrome, also known as PCOS, is a hormonal disease that can affect the ovaries, with a prevalence of around 6.5% of women of reproductive age.3 Diagnosis is when two or more of the following three criteria are met: presence of irregular menstrual periods, excess androgens (greater than typical amounts of male hormones), or ovarian cysts. Hirsutism (undesired male-pattern type hair growth in women) may be an additional symptom, but is not diagnostic criteria.2
PCOS has also been epidemiologically linked to type 2 diabetes (T2D), in which in one study by Gambineri et al., it was found that of their studied patients with PCOS, 15.7% had impaired glucose tolerance.4 In another study, by Moran et. al, there was increased prevalence of T2D in women with PCOS, with odds ratios of 4.43, and 4.00 when BMI-matched.5 This epidemiological link between PCOS and T2D may be due to insulin resistance presenting in both diseases.1
Because of this epidemiological link between PCOS and T2D, patients with PCOS are at risk for developing T2D, and dietitians treating patients with PCOS should also consider strategies for diabetes prevention.
In one study, women with PCOS consumed three 16-day long eucaloric diets, each diet being separated by a 3-week washout period. It was found that in general, fasting insulin blood levels were lower in diets with lower dietary carbohydrate intake (43% vs 56% total kCal), and may be able to improve endocrine and reproductive function in the future for women with PCOS.3
A study done by researchers at Stanford University compared results between two isocaloric diets, both given to obese women with PCOS and insulin resistance. One of the diets was standard (60% carbohydrates/25% fat) and one was low carbohydrates/high unsaturated fat (40% carbohydrates/45% fat), both of which the remainder was composed of 15% protein and <7% saturated fat. After three weeks on each diet, daylong glucose, insulin, and fasting lipids were measured in each participant.
It was discovered that although daylong glucose was not significantly different between the two diets, insulin concentrations in the women on the low carbohydrates diet had significantly lower daylong insulin levels (30% lower,) along with some observations of beneficial changes to their lipid profile levels (observations of lower low-density lipoprotein cholesterol.) As a result, this dietary intervention of low carbohydrates and high unsaturated fat may be a potential dietary treatment for patients with PCOS in preventing the onset of T2D.7
Dietitians can play an important role in the management of PCOS, and strategies are needed to increase referrals of patients with PCOS to dietitians. In addition, sound advice for dietary lifestyle choices for the prevention of type 2 diabetes in PCOS patients is an important part of patient care.
References:
- Barber, T. M., & Franks, S. (2012). The link between polycystic ovarian syndrome and both type 1 and type 2 diabetes mellitus: What do we know today? Women’s Health.
- Boyle, J., & Teede, H. J. (2012). Polycystic ovary syndrome: An update. Australian Family Physician, 41(10), 752-756.
- Douglas, C. C., Gower, B. A., Darnell, B. E., Ovalle, F., Oster, R. A., & Azziz, R. (2006). Role of diet in the treatment of polycystic ovary syndrome. Fertil Steril.
- Gambineri, A., Pelusi, C., Manicardi, E., Vicennati, V., Cacciari, M., & Morselli-Labate, A. M. (2004). Glucose intolerance in a large cohort of Mediterranean women with polycystic ovary syndrome. Diabetes, 2353-2358.
- Moran, L. J., Misso, M. L., Wild, R. A., & Norman, R. J. (2010). Impaired glucose tolerance, type 2 diabetes and metabolic syndrome in polycystic ovary syndrome: A systematic review and meta-analysis. Human Reproduction Update, 16(4), 347-363.
- PCOS (Part 2) [Image]. (2017). Retrieved from https://commons.wikimedia.org/wiki/ File:PCOS_(Part_2).png
- Perelman, D., Coghlan, N., Lamendola, C., Carter, S., Abbasi, F., & McLaughlin, T. (2017). Substituting poly- and mono-unsaturated fat for dietary carbohydrate reduces hyperinsulinemia in women with polycystic ovary syndrome. Gynecological Endocrinology, 33(4), 324–327. https://doi.org/10.1080/09513590.2016.1259407
- Polycystic ovarian syndrome (PCOS). (2014). Retrieved from www.diabetes.org/living-with-diabetes/
Image: A medical illustration depicting PCOS by Bruce Blaus is licensed under CC BY-SA 4.0.